
Fertility
Male Fertility Crisis: What Global Trends Tell Us
Eloise Edington | 1 Dec 2021

Reports of a “population crisis” because male fertility is on the decline make for bleak reading. So we’ve turned to our The Ribbon Box partner, Legacy, to find out: are male fertility rates declining and, if so, why is male fertility dropping?
Legacy is a digital fertility clinic offering at-home sperm testing and freezing, as well as the tools to improve sperm quality (read their profile here).
Today, Legacy’s Alecia Eberhardt-Smith reports on the global trends of male fertility and offers suggestions on how to improve sperm quality and quantity.
Over to Alecia
You may have heard in recent years about the so-called “male fertility crisis” (also dubbed, creatively, as “spermageddon”). How much of this is fear-mongering? And, if spermageddon is real, what could be causing the drop in male fertility?
Fertility is decreasing globally
A population’s “fertility” is measured by the number of children born per adult woman. According to the US Population Reference Bureau’s 2021 Data Sheet, fertility is down in low-, middle-, and high-income countries.
The United States reached an all-time fertility low of 1.7 children per woman (or 55.8 children per 1,000 women) in 2019. Provisional data suggests that – likely due to the COVID-19 pandemic – birth rates declined another 4% in 2020.
Similar trends can be seen in Europe. Fertility rates in the United Kingdom have been declining for over a decade, currently hovering around 1.6 children per woman. Not a single country in the European Union has a fertility rate over 2.0, the “replacement rate”. This means that, eventually, the population will shrink.

Why is this happening?
There are many possible reasons for people having fewer children. In general, as healthcare (and access to contraceptives) improve, people will have fewer children by choice. Women also tend to have fewer children when they have more educational and occupational opportunities.

There are other socioeconomic factors that affect people’s family-planning choices. For example, in the United States, nearly 60% of childless millennials say they’ve put off having kids (or have chosen to forgo parenthood altogether) in part because it’s too expensive to raise children. Almost half say they’re worried about the political and economic climate; 34% are worried about the actual climate.
For those who live in the US, you can receive $65 off an at-home sperm-testing kit by entering code DADLIFE65 at checkout. Find out more here.
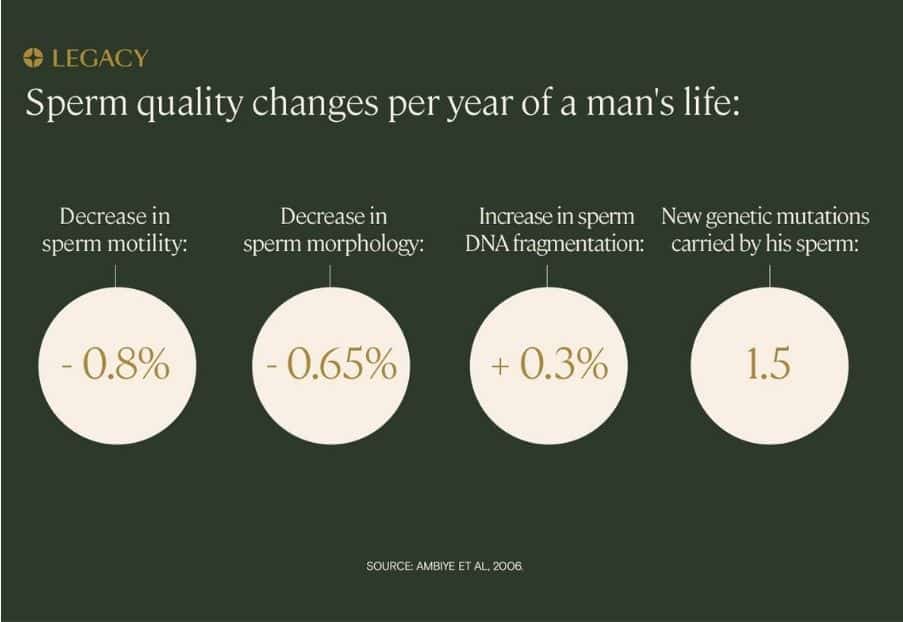
As parental age increases, fertility rates decrease
In most high-income countries, such as the US and UK, increasing parental age is likely also affecting fertility rates.
The average age of a first-time American mother in 1970 was 21; in 2014, it was 26. Paternal ages have increased in the US, as well: in 1972, the average age of first-time fathers was 27. Now, it’s around 31 years old—and nearly 1 in 10 fathers are over 40 at the birth of their first child, according to a 2017 study.
In the UK, age at first birth has been steadily increasing since the 1970s. The average age of first-time mothers has risen from 26 to around 30; for fathers the average age is 33.
Both partners’ ages are important fertility factors. Increased parental age is associated with increased chance of infertility, longer time to pregnancy, and fewer children overall, especially after age 35 for women and age 40 for men.

Sperm counts and quality in decline
But it’s not just birth rates that are decreasing. It appears that the scientific markers of male fertility, namely sperm count and quality, may be on the decline as well.
The idea that we’re approaching “spermageddon” was first presented in a 1992 study looking at over 50 years of semen analysis data – 61 studies of nearly 15,000 men. Researchers found that average sperm concentration had declined by over 50%.
Then, a much-publicized 2017 study looked at changes in average sperm concentration between 1973 and 2011. The study was impressive; it aggregated sperm concentration data from 185 studies of 42,935 men. The research found again that sperm concentration had declined by 52.4%, and total sperm count by 59.3%, in the time period studied.
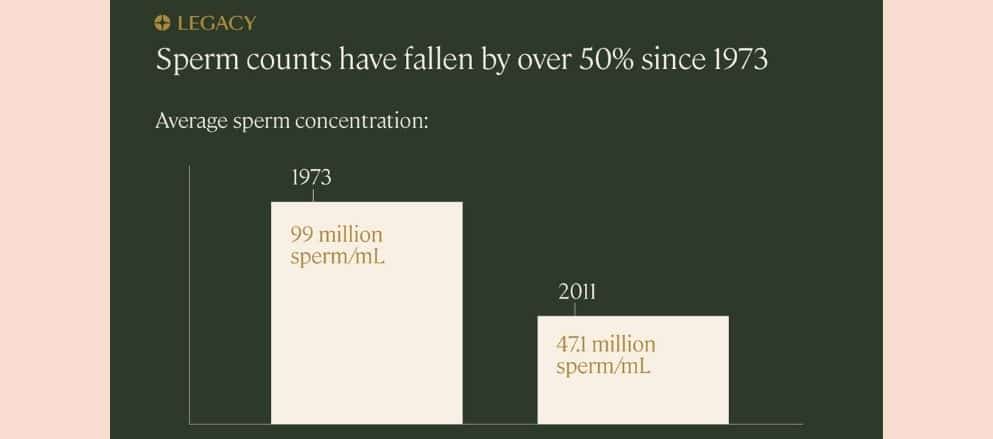
This drop was significant and alarming enough to prompt the researchers to conclude that, due to the “significant public health implications of these results,” further research was “urgently needed”.
In 2021, New York-based researchers completed another study of sperm count over time, this time looking at sperm donors in the United States (176,706 samples from 3,532 donors). Similarly, this study found a significant decline in average sperm concentration and motility (how well sperm are “swimming”) between 2005 and 2021.
In her book Count Down, researcher Dr. Shanna Swan estimates that, if we follow the curve of the sperm count decline documented in the 2017 study, we’re on track to have an average sperm count of zero by 2045.
Semen analysis kits from Legacy are the most advanced at-home testing kits. They analyse the five key factors of sperm health, including assessment of sperm DNA fragmentation, which no other at-home semen testing kit offers.
Use code DADLIFE65 at checkout for $65 off your testing kits, if you live in the US.

Controversy in research
There are some experts who are less convinced that we’re in a full-blown crisis. Firstly, some of the research used in the 2017 meta-analysis was missing some data points, like the men’s age, that may have helped explain discrepancies in semen analysis results over time.
Secondly, the samples examined were primarily from white, Western high-income countries, so the results may not be applicable globally. In fact, the results found that fertile men from non-Western countries actually experienced an increase in sperm concentration over the 40 years studied.
Some researchers point out there is some natural variability to sperm counts, which may also help explain the change. And even after dropping 52%, average sperm concentrations were still fairly high. In 2011, average sperm concentrations were just shy of 70 million sperm/mL of semen; anything over 15 million/mL is considered normal.
Finally, there have, of course, been changes and improvements since 1973 in the way semen analysis is performed and reported. As one andrology (sperm health) expert noted, it may simply be that earlier scientists were over-counting sperm.
Still (especially with the addition of the 2021 study indicating a continued decline over the past 16 years) there’s enough evidence to suggest that men in Western countries are experiencing at least some impairment of sperm count and quality.
Possible causes of male fertility decline
So, why is this happening? The short answer: we don’t really know. There are a number of possible hypotheses, but we’ve yet to pinpoint the exact cause for global male fertility decline.
- Lifestyle: exercise, bodyweight, sleep
It won’t surprise most people to hear that, in the Western world, our lives are more sedentary than ever before. A sedentary lifestyle has been shown to be negatively correlated with sperm health. Similarly, about two-thirds of the US and the UK are overweight or obese, a higher number than ever before; excess body weight is linked to lower semen parameters and reproductive hormone levels.
Plus, modern adults aren’t sleeping very well. Today, over 35% of working adults in the US don’t get enough sleep, up from 30% in 2010. Sleeping less than 7–8 hours per night has been correlated with lower markers of male fertility.
However, it’s unlikely to be solely lifestyle factors that fully explain the global decline in sperm count. It turns out that household dogs are also experiencing a significant annual decline in average sperm count, and researchers found high concentrations of certain chemicals in their testes.
- Chemical exposure
As Dr. Swan argues in Count Down, there’s some good evidence that declining sperm count and overall fertility may be linked to our exposure to endocrine-disrupting chemicals (EDCs). EDCs are chemicals that interfere with the endocrine – or hormone – system, and can be found in many plastics, pesticides, and household products.
One example is phthalates, a class of chemicals used to make plastic more flexible and durable. Phthalates can be found in vinyl flooring, carpeting, and personal care products. Dr. Swan’s research has concluded that phthalate exposure throughout a person’s life, through ingestion or skin contact, is associated with decreased semen parameters. (Phthalates were also what researchers found in the testes of the adult dogs they studied.)
Other EDCs include BPAs, often found in plastic water bottles; PFAS, used in non-stick cookware and firefighting foam; and glyphosate, the active ingredient in Round-Up and other pesticides. These and other endocrine disruptors have been repeatedly linked to lower sperm count and quality and increased DNA damage in sperm.
Legacy Chief Medical Officer Dr. Ramy Abou Ghayda has also studied the impact of EDCs on sperm. His research has looked at the impact of exposure to organochlorine pesticides, associated with lower semen volume and sperm motility. He’s also studied the effects of bisphenol S (BPS), a common component in plastics, envelopes, boarding passes, glues, and many other everyday products. BPS is associated with poorer semen parameters, despite being marketed as a “safe” alternative to BPA.
Most modern men are exposed to these chemicals daily. Once endocrine disruptors enter the environment, they never completely break down, leading some researchers to call them “forever chemicals.” Plus, EDCs actually accumulate in fat and body tissues, so even if each individual exposure might be at a “safe” level, concentrations of these chemicals in our bodies can build up over time.
How can I protect my fertility?
Unfortunately, these chemicals are part of our day-to-day lives. Despite their clear detrimental effects, it might be hard to avoid or eliminate them completely — they’re found everywhere from food packaging to drinking water to soil.
Steps to reduce your exposure to EDCs:
- Avoid plastic and flame retardant materials, especially in food packaging, children’s toys, furniture, and home flooring.
- Choose frozen, fresh, or dried foods over canned, as cans often contain BPA or BPS lining.
- Drink from the tap instead of bottled water (to reduce plastic exposure), and use a water filter to reduce EDCs in your drinking water.
- Check the ingredients of your household cleaning products and personal care items, and consider reducing how many of these you use on yourself and/or your kids.
While it’s good to eliminate the exposures you can identify, a man who hopes to improve his fertility shouldn’t stop his efforts after switching to glass food containers and “clean” household products. Smoking cessation, weight loss, exercise, and supplementation with antioxidants have all been shown to have a positive effect on the quality and quantity of an individual’s sperm, and may help counteract the negative impact of environmental exposure.
To fully understand your sperm health, check out at-home male fertility testing.
If you live in the US and want to receive $65 off a sperm analysis kit, enter code DADLIFE65 at checkout.
We love the depth and breadth of this research and thank Alecia and Legacy for their expertise. To discover similar content about male (in)fertility, subscribe to FHH’s weekly newsletter.









