Navigating a septate uterus with pregnancy – what a doctor wants you to know
What does it mean if you have a septate uterus? Can you have a normal pregnancy, and what’s the best advice if you’re looking to start or grow your family?
You’ve found part three of our Mullerian anomaly series. In part one, we explored the different Mullerian anomaly uterus types in detail, so if you haven’t read that yet, check it out first to understand how different anomalies compare!
Now, let’s unpack how to navigate a septate uterus with pregnancy – pulling in the expert perspective from Samantha Pfeifer, M.D.
What actually is a septate uterus?
A septate uterus is a Mullerian anomaly (also known as a uterine anomaly) that many people only discover when trying to conceive or during an early pregnancy scan.
Dr Pfeifer explains: “This is a uterus with an outer single body, but inside there is a septum or fibrous tissue that divides the inner cavity of the uterus into two. This can either be partial or less commonly a complete septate configuration.
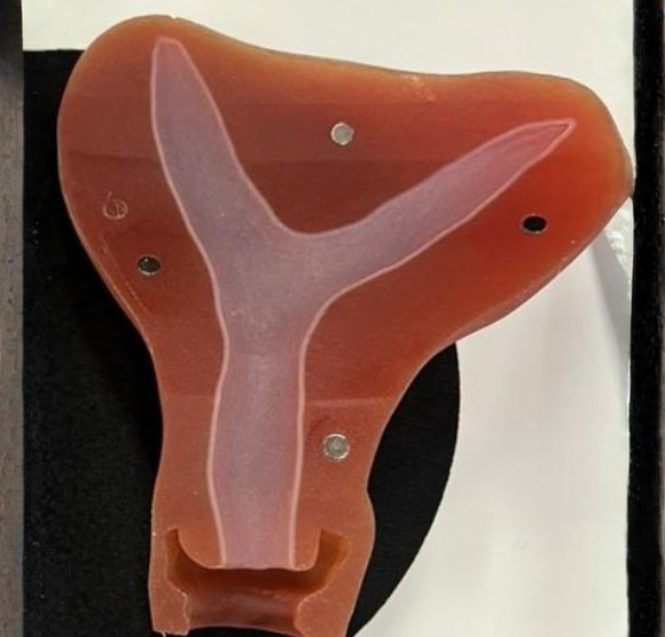
A septate uterus is not to be confused with other similar types of Mullerian anomaly, which include:
- Bicornuate – A heart shaped uterus on the outside, and two separate cavities on the inside
- Unicornuate – A uterus with a single-sided, small banana shape with one fallopian tube and ovary attached on that side and a fallopian tube and ovary on the other side
- Didelphys – Two separate outer bodies that look like two separate uteruses with two cavities, two cervixes and two vaginal canals
Can you get pregnant with a septate uterus?
If you’re wondering can you get pregnant with a septate uterus, the short answer is yes.
“You can get pregnant with a septate uterus. In fact, almost all of the Mullerian anomalies are not associated with infertility and whilst septate uterus is often diagnosed during early miscarriage via ultrasound, it is not clear whether early miscarriage itself is caused by septate uterus” Dr. Pfeifer explains.
This means that having a septate uterus usually doesn’t stop you from conceiving, and most people with this condition will become pregnant naturally without interventions.
Can you have a normal pregnancy with a septate uterus?
In short, yes you can – but there are a few considerations.
“Septate uterus is associated with a slightly higher risk of preterm delivery, premature birth and breech presentation, and pregnancy may need care from a high-risk obstetrician and frequent check ups.
But, with a septate uterus, a minor surgery to remove the septum can be done prior to planned pregnancy, and here we see that there’s an improvement in pregnancy outcomes,” Dr. Pfeifer explains.
In other words, while a septate uterus may introduce some extra pregnancy considerations and specialist monitoring, surgical correction can improve outcomes, making a healthy pregnancy achievable with some careful planning.
Is surgery always recommended?
No, surgery isn’t always necessary with a septate uterus.
“You can get pregnant without surgery. Most with a septate uterus won’t have any difficulties getting pregnant, or carrying a pregnancy to term.” Dr. Pfeifer says.
The bottom line? Surgical intervention is often considered on a case-by-case basis, particularly if someone has experienced recurrent pregnancy loss or complications in prior pregnancies.
Hysteroscopy for septate uterus, explained
One common procedure to address this condition is hysteroscopy for septate uterus.
This minimally invasive surgery is safe and effective, and allows a gynecologist to remove the septum.
The procedure is typically done as a day case, and recovery is often quick, with most people resuming normal activities shortly after.
Some studies show that it could help improve fertility outcomes and reduce risks associated with pregnancy.
Been diagnosed? 4 steps for navigating a septate uterus with pregnancy planning
Dr. Pfeifer advises a clear, structured approach: “The first thing that should be done is to clarify your diagnosis. This involves seeking care from a specialist gynecologist, and seeking appropriate imaging – such as a 3D ultrasound or an MRI.
Accurate diagnosis is key because this type of uterine anomaly can be confused with other uterine anomalies. Septate uterus is unique as it may simply be corrected surgically to improve reproductive outcomes.
Other anomalies, such as a bicornuate uterus or didelphys uterus, are usually not correctable but can be managed carefully during pregnancy by a high-risk obstetrician.”
Here’s a step-by-step to-do list to save for later:
- Confirm your diagnosis: See a specialist gynecologist who is experienced in Mullerian anomalies.
- Get detailed imaging: Ask for a 3D ultrasound or MRI to understand whether your septum is partial or complete.
- Discuss surgical options: If you have a septate uterus, talk about hysteroscopic removal of the septum and how it could improve pregnancy outcomes.
- Plan pregnancy monitoring: Ensure your obstetric care team knows about the anomaly so they can monitor.
Taking these steps ensures that your pregnancy will be monitored appropriately and that any potential risks are managed proactively.
Liked this feature? Watch this next: Charlie’s story: an MRKH diagnosis, crossing the pond and a surrogacy family-building journey