4 Mullerian anomaly uterus types, explained by an MD
If you’ve come across the term Mullerian anomaly online, or even been told you have one yourself, you might have more questions than answers. And, from treatment options to pregnancy success, there is some information out there.
However, it tends to be targeted towards medical professionals rather than patients, and, with more research into these rare conditions still needed, what is available can be somewhat fragmented and, well, just a bit confusing.
This kind of specific guidance always comes best from the experts, so to start the year we’re kicking off a three part mini-series with Samantha M. Pfeifer, M.D, a reproductive endocrinology and fertility specialist at Weill Cornel in New York, and a leading expert in Mullerian anomalies, to cover off some of the most frequently-asked queries.
Here in part one, we ask Dr. Pfeifer what a Mullerian anomaly of the uterus actually is, as well as the main types to know, and their key differences.
In parts two and three, we’ll be providing more detailed guidance on how certain individual anomalies can affect fertility and pregnancy specifically.
First up though: the basics.
What is a Mullerian anomaly?
“A Mullerian anomaly is a rare variation of the development of the uterus, and there’s a spectrum of these anomalies ranging from the absence of a uterus all the way to what appears to be two uteruses, cervixes and vaginas, and everything in between,” says Dr. Pfeifer.
These variations happen before birth, when the Mullerian ducts (which form the uterus, cervix, fallopian tubes, and upper vagina) don’t develop or fuse in the typical way.
This results in different uterine shapes and structures, and are currently grouped under the ASRM Mullerian anomalies classification 2021.
Mullerian anomalies may present during adolescence with primary amenorrhea – lack of first menstrual period, or intermittent lower abdominal pain associated with lack of first menstrual period, or with severe pain with menstruation. But many mullerian anomalies have no symptoms and are first discovered during imaging, fertility investigations, or pregnancy care.
What is a double uterus, and is it the same thing as a mullerian anomaly?
One of the most searched questions is what is a double uterus?
This might paint quite a clear visual for many of us, but in medical terms, it’s not actually a single diagnosis.
“A double uterus is absolutely real, and can refer to many different shapes of uterine anomalies, including a septate uterus, a bicornuate uterus, and a uterus didelphys. Each one is very separate and distinct, and the term ‘double uterus’ really does not explain the exact variation, so should not really be used,” says Dr. Pfeifer.
Basically, accurate diagnosis and categorization is really important, as different anomalies not only look different, but have different implications for pregnancy and are managed in very different ways.
Mullerian anomaly uterus types, visualized
1. Septate uterus
A separate uterus is where the outside of the uterus appears normal, but is split into two on the inside.
This happens when the two Mullerian ducts that create the uterus form and fuse, but the central dividing wall remains.
Dr. Pfeifer explains: “This is a uterus with an outer single body, but inside there is a septum or fibrous tissue that divides the cavities of the uterus into two. This septum can be partial, meaning only affecting the uterine cavity, or complete with the septum extending through the cervix and even vagina resulting in two separate vaginal cavities.”
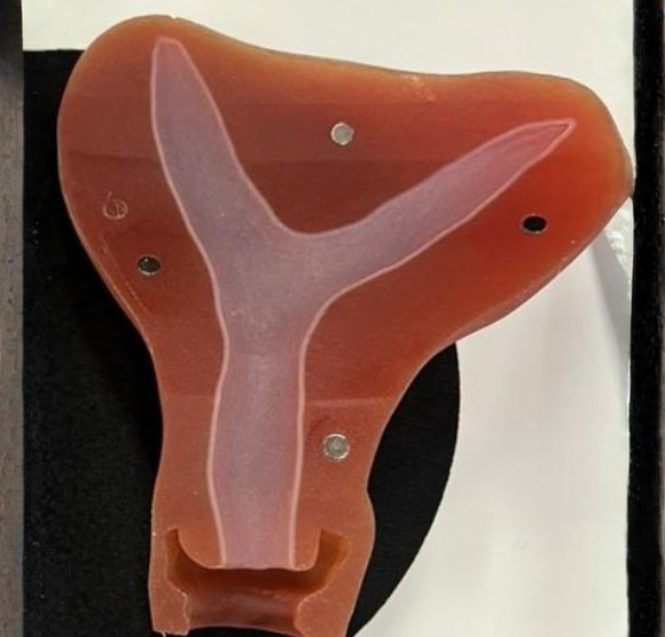
The septum can affect how an embryo implants and how the uterus expands during pregnancy.
This is one of the few Mullerian anomaly uterus types that can often be corrected surgically ahead of pregnancy.
Read more: Navigating a septate uterus with pregnancy
2. Bicornuate uterus
A bicornuate uterus forms when the Mullerian ducts partially fuse, creating a single uterus with a noticeable indentation at the top.
“This is a heart shaped uterus on the outside, with two separate cavities on the inside,” Dr. Pfeifer explains.
This anomaly is not typically corrected with surgery, but many people carry pregnancies successfully with careful specialist monitoring.

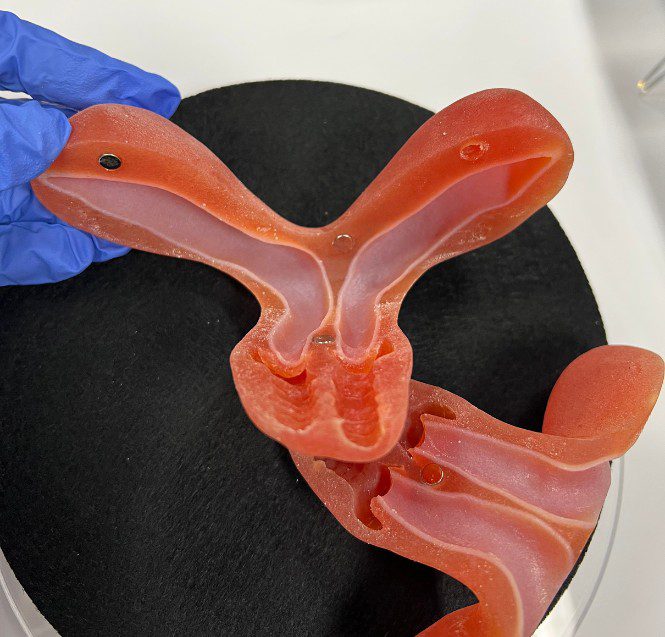
3. Unicornuate uterus
A unicornuate uterus has a single, one-sided banana shape, and forms when only one of the two Mullerian ducts develops.
“The unicornuate uterus is typically on one side of the pelvis and is connected to a fallopian tube on that same side. On the other side there may be a small non-functional under-developed uterine remnant and fallopian tube. Sometimes this remnant may contain endometrial tissue and cause pain,” says Dr. Pfeifer.
The uterus is smaller than average, which can affect how pregnancy progresses.
Fertility is often possible, but pregnancies are usually monitored by a high-risk obstetrician.
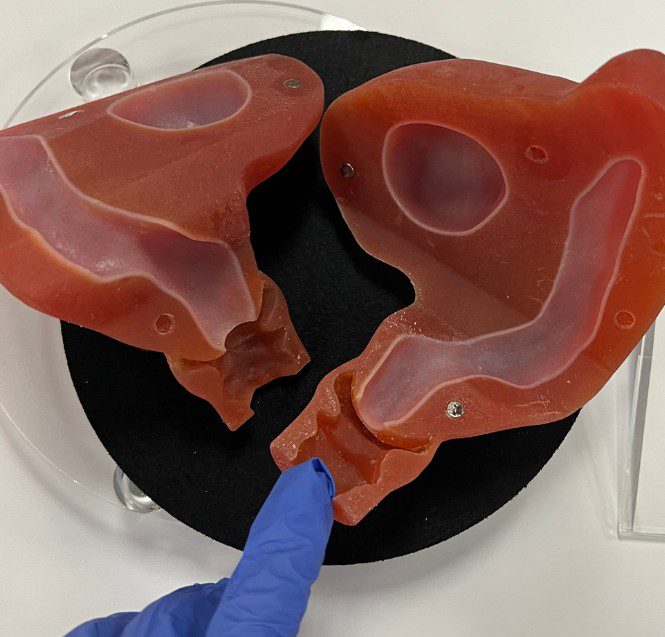
4. Uterus didelphys
A uterus didelphys is the anomaly most people imagine when they think about what a double uterus looks like.
“Here we’ll typically have two separate outer bodies that look like two separate half uteri with two endometrial cavities, two cervixes and two vaginal canals,” Dr. Pfeifer explains.
Each uterus functions independently, and pregnancy can occur in either one. Fertility is usually not affected, but pregnancy care needs to be completely individualized.
Other Mullerian anomalies
The ASRM guidance has further categories and treatment routes for anomalies that don’t fit into the above, including:
- Mullerian agenesis – Also known as Mayer-Rokitansky-Küster-Hauser syndrome (MRKH), this is a complete absence of the uterus. In this case, there are big consequences for fertility as it is not possible to carry a pregnancy, but biological children are possible through other routes.
- Other complex anomalies – A category for cases that involve combinations of anomalies, or those that simply do not fit into the other specific categories.
Read more: These are the top reasons someone might opt for surrogacy (& they’re all so valid)
Your key takeaways
Understanding Mullerian anomaly uterus variations is key, especially when it comes to managing fertility and pregnancy expectations. Here’s what to remember:
- ‘Double uterus’ is a broad term and doesn’t correctly indicate the exact type of anomaly.
- Structural differences range from septate and bicornuate to unicornuate and didelphys, as well as complete absence, as in MRKH.
- Most anomalies do not prevent pregnancy but may require monitoring for preterm labor or other complications.
- Some anomalies, like a septate uterus, can be corrected surgically to improve pregnancy outcomes.
- Early diagnosis with imaging, such as 3D ultrasound or MRI, is crucial for supporting fertility and family planning.
View this post on Instagram
Looking for support?
If you’ve been diagnosed with a Mullerian anomaly, it can help to connect with trusted resources for guidance and support. Here are some options to explore:
- Browse our own library of shared stories on TRB – from an MRKH surrogacy journey to IVF with IVF with Uterine Didelphys, it’s here
- RESOLVE: The National Infertility Association – offers support groups, educational resources, and guidance for anyone navigating reproductive health
- American Society for Reproductive Medicine (ASRM) – provides patient-friendly information on Mullerian anomalies, fertility, and treatment options
- MRKH Connect – peer support and education for women with MRKH or related uterine anomalies
- Society for Women’s Health Research (SWHR) – resources on reproductive health and conditions affecting women’s fertility
Connecting with these resources can help you better understand your diagnosis, explore treatment options and find support from others who’ve been through similar experiences.
Got more questions? You can also reach out to Dr. Pfeifer here – she’s currently accepting new patients at Weill Cornell in New York.






