Embryo grading – your top questions answered

Embryo grading and success rates
It’s a fertility truth that when it comes to blastocysts, embryo grading and researching success rates, Google isn’t always a helpful go-to. Before you get lost in a sea of results, research and second guesses, back up and hear from Danielle Breen, Laboratory Manager at TFP Thames Valley Fertility.
With second-to-none expertise across every one of their UK-based clinic network, you’re in the safest hands with this fantastic team. Here are the UK’s top-searched embryo grading and success rates queries, answered.
Over to Danielle Breen.
How do embryologists grade embryos from A to D, or 1-5?
Embryo grading is split into different development stages:
- Cleavage (Days 2-3), and
- Blastocyst (Days 5-6)
Although the principle of what is assessed/graded is universal, the grading systems can vary between clinics. Some clinics may use numbers to assign the grade of the embryo, while others use letters, and some systems even use both.
What do we mean by cleavage stage grading?
As an embryo divides (cleaves), the cells inside get smaller, like taking a biscuit and breaking it in half, and then in half again. Cleavage stage grading is based on how many cells there are in the embryo, how regular they are in size and if each division has been a clean break, without fragments breaking away.
Back to the biscuit comparison, a good division would be being able to break the biscuit into two equal halves, without any crumbs breaking off. Typically, Cleavage stage grading is done on Day 3 of development, unless there are indications or concerns to look at the embryo earlier. By Day 3 we’d hope to see at least six cells in the embryo, with minimal or no fragmentation.
And what is blastocyst stage grading?
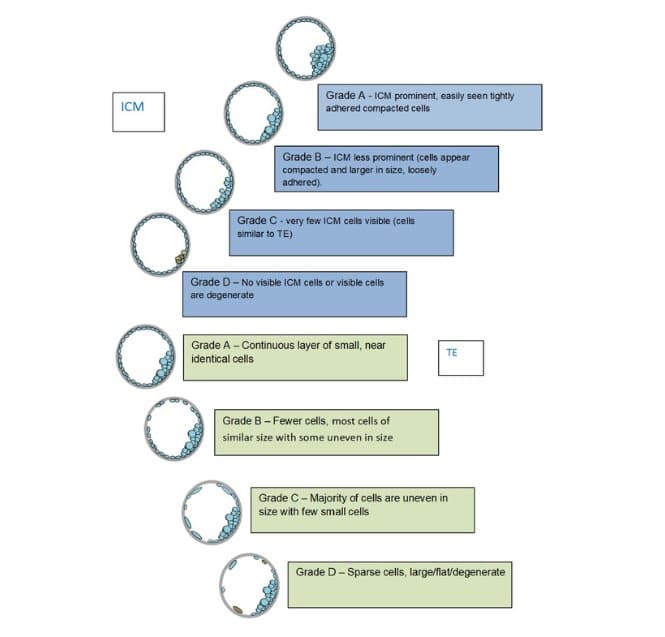
Blastocyst is the name given to embryos that have made it to the correct developmental stage for Day 5/6. By this stage the cells are much smaller and higher in number. The focus of grading is no longer to count the number of cells, but to identify two distinct cell populations.
The first is a tight ball of cells, called the inner cell mass (ICM). This group of cells would go on to form the baby in a successful pregnancy. The other is a flattened layer of cells that create an outer sphere, called the trophectoderm epithelium (TE), this group of cells would go on to form the placenta.
The central area is now filled with fluid, called the blastocoel, which works to expand and stretch the total size of the blastocyst. As the blastocyst grows in total size, the shell around the embryo thins and will eventually reach a breaking point, from which the cells can hatch out. Blastocyst stage grading takes into account all of these factors, the expansion status (how thin the shell has become and if it is hatching yet), the number of cells in the ICM and TE, and whether these cells look healthy.
What is ‘normal’ embryo development?
Embryo development can be visualised as a series of checkpoints.
Starting at fertilisation, then making the first division and then following this division pattern, so that each cell divides again and again (i.e. 2 to 4 to 8 cells). The Day 3 checkpoint is one of the most crucial, with only around half of all embryos making it to the blastocyst stage, on average.
What are the signs of an abnormal embryo?
Grading and embryo development alone aren’t enough to determine whether an embryo is normal or not. In fact, we know from embryo biopsy that some genetically abnormal embryos can still make good quality blastocysts.
With some of the developmental abnormalities we observe, these do not always correlate with the embryo itself being abnormal. The list below sets out some abnormalities that may be observed, but it’s important to note that some of these embryos could still go on to make healthy pregnancies and babies:
- Multinucleation – when the cells contain more than 2 nuclei
- Reverse cleavage – after a cell division has been completed, the step is reversed and the cell re-joins, i.e. 3 cells go back to being 2 cells
- Direct cleavage – when a cell breaks into 3 or more, rather than in half
- Failed cleavage – when a fertilised egg fails to divide at all
- Failed to reach blastocyst – when an embryo doesn’t move past the day 3 cleavage stage
- High fragmentation levels – when there is high cellular mass wasted/lost, due to by poor cell divisions which create fragments
- Vacuoles – when small fluid-filled sacs are present in the egg or embryo
At which grade(s) are embryos ready for transfer, freezing or biopsy?
Most clinics have now moved towards blastocyst stage utilisation. Only approximately half of embryos have the ability to make a blastocyst. So, embryo selection and potential for a pregnancy is already higher simply by ensuring the embryos have moved through this natural Day 3 checkpoint. The stage at which a blastocyst can be used varies slightly, depending on the procedure.
Transfer
We’ll transfer any stage of blastocyst that can be confirmed as moving through the Day 3 checkpoint. This includes very early-stage blastocysts that are still compacting or only starting to cavitate. Following transfer, the blastocyst will still have some time to continue developing in the womb before it needs to have implanted.
This is on the basis that we often see big changes in blastocyst expansion status over a few hours in the lab, and the hope that if this is all a patient has available, theirs will also continue to develop.
Freezing
Our criteria are that only fully-developed blastocysts – with at minimum an average/borderline grade for the ICM & TE – can be frozen. These embryos have the best chance of surviving the freezing and thawing procedures. And, we can then guarantee that frozen pregnancy rates are as high as fresh pregnancy rates, based on knowing the quality of the embryos frozen.
Biopsy
Here, our criteria are that only full or expanded blastocysts can be biopsied. This is because you must be able to clearly differentiate the ICM and TE, and be able to safely remove approximately 5 cells from the TE without causing too much disruption to the remaining blastocyst. If a blastocyst is biopsied too early, the TE cells will still be quite large – and harder to remove.
What do we mean by embryo hatching?
Hatching – or ‘assisted hatching’ – is the process of introducing a small hole in the zona pellucida (ZP) shell around the embryo/blastocyst. It can be performed for different reasons:
1 – In preparation for embryo biopsy
This can be done prior to Day 5, to encourage the TE layer of cells to start herniating through the hole to make the biopsy easier
2 – As part of the thawing process
This can be done as part of the thaw, where the freezing process is thought to have toughened the ZP
3 – For increased zona thickness, or to improve pregnancy potential
This can be done when the ZP is looking extra thick. However, with nearly every clinic using blastocyst culture in 2023, it’s now rare to use assisted hatching for ZP thickness. This is because forming a blastocyst naturally starts to thin and stretch the ZP.
How accurate is embryo grading for predicting IVF success?
Although we can track embryo development through the expected checkpoints, embryo grading has its limitations. Very sadly, we see perfect, top-grade embryos fail to create pregnancies and can be surprised when those we graded as poorer-quality have led to successful pregnancies and healthy development.
You could see grading as being only skin-deep – we cannot predict if the embryo is viable, genetically, simply by how it looks. That said, we do know that embryos which fail to move through the standard development checkpoints are almost always abnormal.
As an embryo biopsy practitioner, experience has taught me that embryo (genetic) abnormality is often not about the grade.
My focus for fresh transfer (without a biopsy) is:
- has the embryo made it through each of the checkpoints, and
- do we have a blastocyst with clear cell populations (ICM & TE) and healthy looking cells in each of these?
If so, then fingers crossed.

Can I influence the grade of my embryos?
Embryo quality factors can be very difficult to pinpoint, and aren’t always something patients can directly influence.
That said, embryos come from two tiny cells – the sperm and egg. So, trying to ensure the starting blocks for development are the best they can be sets the embryo up for the best start.
I recommend focusing on the following:
- improved blood flow and circulation
- a healthy diet and lifestyle (maintaining a healthy weight and exercise routine)
- targeted fertility supplementation (both female and male)
- sufficient sleep
- reducing stress
- minimal or zero alcohol, smoking and caffeine intake
Embryo grading and gender – is there a link?
Sorry to bust a myth, but no!
However, there is some evidence to suggest that male embryos may reach the blastocyst stage faster. That said, in clinics that do embryo biopsy the ratio or male to female normal blastocysts has been reported to be similar between both genders.
In the UK, it’s illegal for a clinic to reveal embryo gender through embryo biopsy techniques.
That’s it! Your top embryo grading questions covered, plus the 101 on success rates and myth-busting. Head to TFP Fertility UK to connect with the amazing TFP Fertility team, and build a plan that’s dedicated to you.


